The standards we demand in mental healthcare
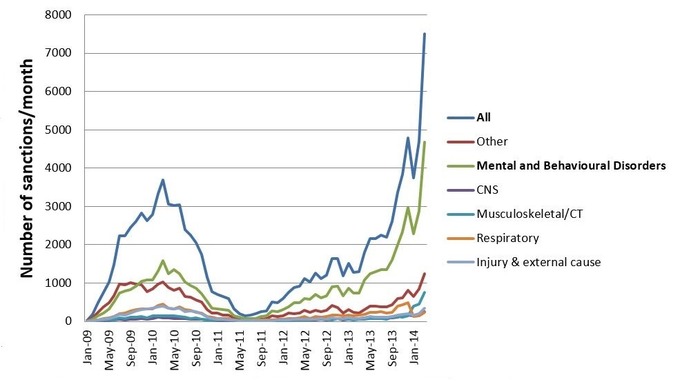
ESA sanctions ranked by disability: Notice that mental illness attracts by far the largest number of sanctions. Yet the UK simply does not support people with mental health problems. Isn’t that the REAL problem?
It is very easy to pre-judge a Parliamentary debate – on any subject – if you know a little about it already. As a carer for a person with mental health issues, This Writer could list off on my fingers the main issues that need to be tackled.
First, I would single out early recognition of the signs that somebody has a mental health problem. So many of the people I know who fell victim to mental issues as adults were already suffering in their childhood and adolescence – but nobody picked up on it. Prevention is better than cure – especially if the only cures available aren’t very reliable.
But we have a Conservative Government that sees everything in money terms but, as the saying goes, knows the cost of everything and the value of nothing. In today’s Parliamentary debate we learned that, on this Government’s watch:
- There has been an increase in the number of patients who report a poor experience of community mental health care.
- More patients have to travel hundreds of miles just to get a bed.
- The number of children being treated on adult wards, against the intention of the Mental Health Act 1983, has risen again this year.
- The number of people becoming so ill that they had to be detained under the Mental Health Acts leapt by 10% in the past year.
- The level of suicides, particularly among men under 45, has been at its highest since 2001.
- There has been a psychiatry recruitment crisis, with a 94% increase in vacant and unfilled consultant posts.
- The Government claims to be increasing mental health budgets, but patients and professionals tell a different story.
- We do not have an accurate picture of spending on mental health in our country since ministers stopped the annual survey of investment in mental health three years ago.
- Many of the statistics that were available previously are no longer available.
- Last year, funding for mental health trusts was cut by 20% more than that for other hospitals.
- In 2011-12, total investment in mental health dropped for the first time in a decade – and in the same year, the Government stopped publishing how much they invest in mental health.
- Last year, 67% of Clinical Commissioning Groups who responded to a FoI request spent less than 10% of their budget on mental health, despite the fact that mental health accounts for 23% of the total burden of disease.
- This year, the Minister for Community and Social Care promised he would ensure that investment in mental health by clinical commissioning groups increased in this financial year in line with the increase in their overall budgets – but more than one in three CCGs were not meeting the Government’s expectation.
- The Conservative Government committed itself to spending £250 million on child and adolescent mental health services this year. There will be a £77 million shortfall on that pledge to spend this year.
- The NHS constitution enshrines our rights to access drugs and other treatments, but it does not extend that right to talking therapies. Recently, the Government consulted on adding a right to psychological therapies to the NHS constitution, but they decided not to include it in its latest version.
- The number of children with a mental health problem who turn up at Accident and Emergency has doubled in recent years.
- One person in prison takes their own life every four days.
- Young people who are self-harming may be told that because they are not suicidal they do not meet the threshold for help.
- People with an eating disorder may be turned away from specialist services because their body mass index is not low enough.
- Too often, mental health problems are ignored, and it is only when they reach crisis point that they receive attention. Recent studies have put the cost of mental ill health to our society at £105 billion a year.
- 75% of people who have mental health problems in working life first experienced symptoms in childhood or adolescence, yet only about 6% of the mental health budget is spent on child and adolescent mental health services. Mental health education is often omitted from the school curriculum owing to a lack of teacher training.
- Poor housing, fuel poverty and neighbourhood factors, such as overcrowding, feeling unsafe and a lack of access to community facilities, can have a harmful impact on mental health.
- These, along with abuse, bullying, trauma, deprivation and isolation, are just some of the levers of mental distress in our communities that we must address.
- The Government’s deep cuts to local authority budgets over the past five years, the additional £200 million in-year cuts to public health and cuts coming further down the line, will impact on our communities and their services, such as libraries, drop-in centres, leisure centres, befriending services, children’s centres and citizens advice bureaux, which support people early on.
- Billions have been slashed from social care budgets and the number of people receiving social care support for mental health has fallen by a quarter since 2009-10, seriously harming mental health trusts’ ability to discharge their patients.
- 70 million working days are lost every year owing to stress, depression and other mental health conditions.
- Mental health problems cost employers in the UK £30 billion a year through lost production, recruitment and absence.
- Across the NHS, staff are concerned about their well-being and that of their colleagues. The NHS staff survey shows that the proportion of staff reporting work-related stress has increased from 29% in 2010 to 38% in 2014.
Those are only a few of the issues identified in the debate today (Wednesday, December 9).
Labour is asking the Government to restore transparency to the murky picture of mental health funding. It is asking Ministers to address the fundamental inequality in our NHS constitution. And it is asking the Government to prioritise prevention and implement a fully cross-departmental plan to prevent mental health problems from developing in the first place.
The Health Secretary, Jeremy Hunt, appeared noncommittal in the debate – preferring to discuss what he saw as successes in mental health care. So let’s keep this list in mind and see how well he, and his government, fare in rectifying these issues in the future.
Join the Vox Political Facebook page.
If you have appreciated this article, don’t forget to share it using the buttons at the bottom of this page. Politics is about everybody – so let’s try to get everybody involved!
Vox Political needs your help!
If you want to support this site
(but don’t want to give your money to advertisers)
you can make a one-off donation here:
Buy Vox Political books so we can continue
fighting for the facts.
Health Warning: Government! is now available
in either print or eBook format here:
The first collection, Strong Words and Hard Times,
is still available in either print or eBook format here:






This is an excellent blog, Mike and a resounding indictment of this government. It’s no good Labour asking – they need to be demanding action on all these. And keeping up the pressure at every single opportunity.
Every single statistic translates into lives of suffering, waste, tragedy and misery unless we can get organised locally in our communities and address these issues. Because they are only going to get worse, far worse with the raft of cuts coming down the line.
Local support groups that take on particular issues and press for resources from the grassroots up and keeping up pressure on MP’s seems to be one good way forward. Because these issues affect the whole family without a doubt.
Another problem – especially for women – is to get a respectful diagnosis and care- for long term life limiting or chronic Illnesses. Not being believed- and this is becoming more, not less common as NHS cuts back on investigation and treatment and DWP refuses to recognise certain illnesses.It is a huge source of mental distress which leads to severe depression and anxiety. I had a diagnosis of MS and in the first 10 years had a GP who insisted that certain ways in which MS manifested for me were “all in my mind” and there was nothing he could do.I suggested eventually that I see a Psychiatrist and he just laughed and said it was a waste of resources.
I should make more of an effort.
I am very aware that many people have similar experiences, which can cause lasting damage and depression. THere is a basic prejudice amongst doctors that treating mental health is not ” real” medicine, which is encouraged by the Government, as well of a sense of shame from those who have mental illnesses.
It’s high time mental health was taking seriously, is something that can affect anyone at anytime!